- Chichester Foot and Ankle
- Foot and ankle conditions
- Treatments
- Foot and ankle referrals
-
Resources
- Sites of foot pain
- Links to other foot and ankle services and resources
- Internal
-
Rehab protocols
>
- Rehabilitation from achiles tendon rupture treated without surgery using VACOped boot
- Recovery from achilles rupture without surgery using VACOped boot
- Rehabilitation from achilles tendon rupture treated without surgery using Boot and Wedges
- Rehabilitation from achilles tendon rupture treated with surgery in Aircast boot and wedges
- Foot and Ankle rehabilitation
|
The consequences of leaving plantar fasciitis untreatedWritten by: MR EDWARD DAWE Published: 05/11/2020 Edited by: CAMERON GIBSON-WATT Plantar fasciitis is an inflammatory condition of the fibrous tissues on the bottom of your foot that connect your heel bone to your toes. It can result in intense pain and discomfort, usually under the heel and around the arch. We spoke to Mr Edward Dawe, a specialist in foot and ankle surgery based in Chichester and Worthing, to understand more about plantar fasciitis and what can happen if you leave it untreated. How long does plantar fasciitis normally take to heal? Plantar fasciitis usually resolves on its own but can be very painful. It can take up to two years to resolve in most circumstances. There is a small subset of people who have the condition very severely, who can have plantar fasciitis in the longer term, for many years. What happens if plantar fasciitis isn't going away? There are a number of other conditions which can mimic the symptoms of plantar fasciitis. If you have any concerns, or if you are suffering severe pain then you should seek treatment. This will usually involve scanning and/or X-rays of the heel to confirm the diagnosis. What happens if I leave it untreated? In most cases, if you leave plantar fasciitis untreated it will resolve on its own. However, some people will have severe pain meaning they need early treatment. Others may have heel pain from other causes such as a stress fracture in the calcaneum (heel bone) or nerve entrapment. What does it mean if the pain is getting worse? If the pain is getting worse, this may mean that the plantar fasciitis is getting worse. However, this could also be a sign that your heel pain is coming from a different cause. If the pain is worsening you should seek help to establish the correct diagnosis before proceeding further. When should I see a doctor? If you are struggling with heel pain then there is no need to wait as often some simple measures can help through your doctor. Similarly, if you have had your symptoms for six weeks or so and they are not improving you should see your doctor. If your foot is swelling or going red you should definitely seek treatment. What treatment do I need for this? There are many different ways of treating plantar fasciitis, but most cases can be managed without invasive treatment. This is by a combination of stretching exercises, changes to your footwear and shockwave therapy. Only a small proportion of patients ultimately come for surgery. Shockwave therapy is a type of pulsed soundwave which I use at the Oving Clinic. This can be done at any stage in the disease process and improves things for a majority of patients. Steroid injections carry a risk of plantar fascia rupture and I tend to avoid them for plantar fasciitis. For severe cases, there are surgeries, of which the most commonly performed in my practice is the proximal medial gastrocnemius release. This is a day-case procedure under local anaesthetic which has a rapid recovery. You can walk on your foot immediately and there is very little restriction on your activity afterwards. Plantar fasciitis resolves rapidly in the majority but can be long-term and severe for a small proportion of people. In this group, getting the right input from a foot and ankle specialist can be invaluable.
1 Comment
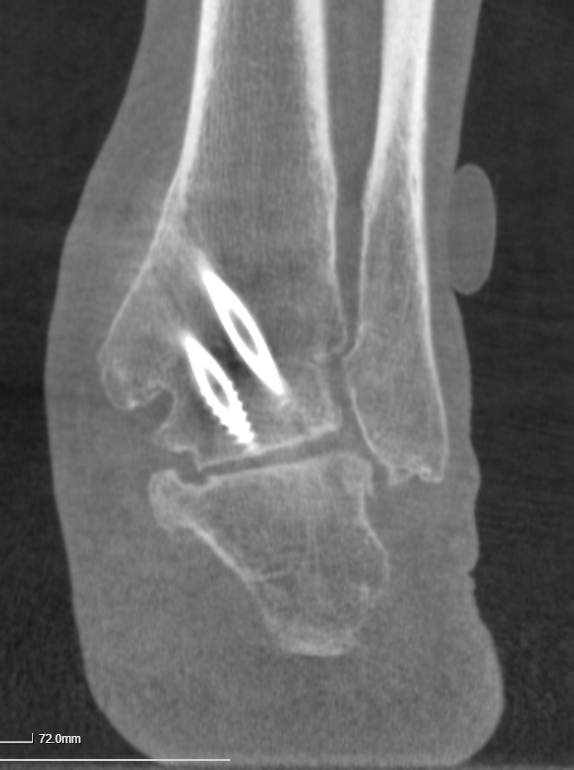
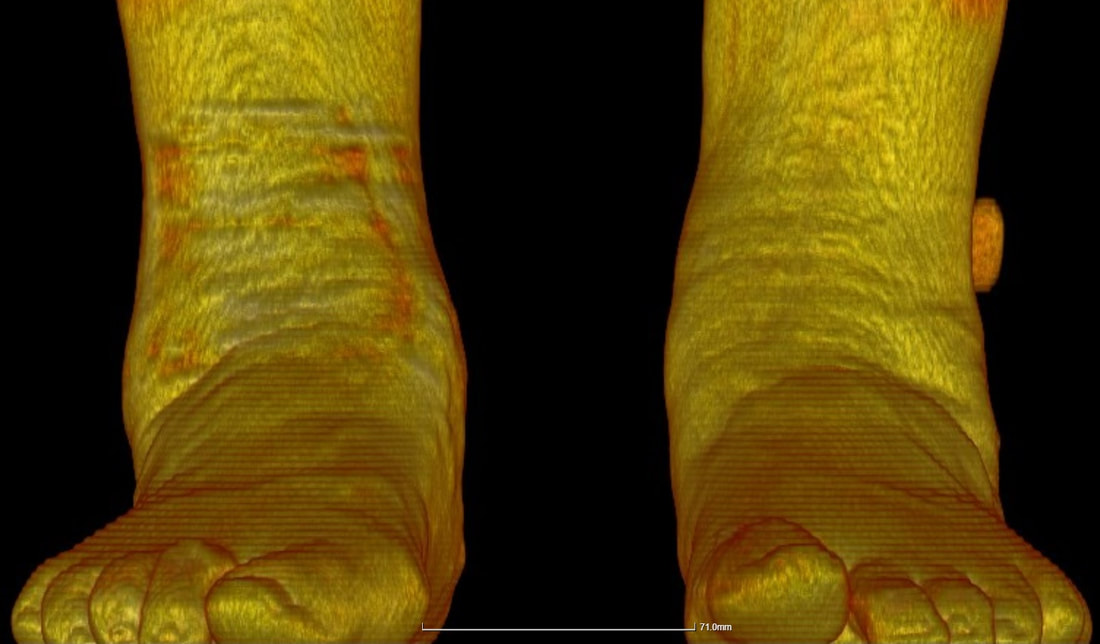 Figure 1: A standing (Cone Beam) CT scan demonstrating the shape and position of a patient's feet. Mr Dawe and the Oving Clinic are pleased to be starting the first Standing CT scanning service based in West Sussex, with a visiting scanner from the Standing CT company. Standing CT scanning has several benefits compared to both conventional X-rays as well as some advantages over both conventional CT scans and MRI. The scanner uses a technique called 'cone-beam CT' scanning which is different to the conventional type of CT scans which re commonly performed in large scanners at major hospitals. The Cone-beam CT scan takes around 1 minute to perform. It uses less radiation than a set of weightbearing Xrays and much less radiation than a CT scan. The major benefit of standing CT is that the foot is imaged in the position in which it is used, i.e. you are standing up to have the scan done not lying down. Conventional CT scans can only show the foot in a resting position where it takes a different shape, arthritic joints might not show-up on a basic scan, but are more easily seen on standing CT. This allows the detection of subtle joint problems which can be difficult to find using other imaging modalities. These scans can help with the understanding of many foot problems such as foot and ankle injuries or fractures, ankle arthritis, midfoot arthritis, bunions, plantar fasciitis and stress fractures, as well as foot deformities such as the painful flat foot and high-arched or cavus feet and toe problems. Most major insurance companies now recognise standing CT as a new image modality and for self-funding patients this scan can be used to reduce the costs of treatment by reducing the use of conventional X-rays and MRI scans. Image 2: A reconstructed Cone Beam CT image showing the hindfoot in a patient with an ankle fusion. This low cost, low-radiation study helped identify and treat the patient's symptoms.
Standing Cone Beam CT scanning can also be used to help decide on treatments for conditions affecting all lower limb conditions including hip and knee arthritis, as well as for the assessment of problems with joint replacements. Furthermore the same scanner can be used for rapidly assessing hand and wrist problems such as injuries or arthritis. USA Visitation - Arthrex - Coetzee Mr Dawe visited the USA in February 2019. He visited the world renowned Dr J Chris Coetzee for a surgical visitation at the Egan Orthopaedic Centre, part of Twin Cities Orthopaedics and joined with the Minnesota Vikings. He then was one of the first UK surgeons to visit the Arthrex facility in Naples Florida in order to spend time in their new surgical development centre. Thanks to Dr Coetzee and to Arthrex for a most informative and useful trip.
A small team of researchers including Mr Dawe have won first prize for their research presentation at the 2018 British Orthopaedic Foot and Ankle Society Meeting. The research used a zero-gravity treadmill (a treadmill which blows air at your legs and can simulate you weighing less, all the way to being completely weight-less) in order to demonstrate the benefits of weight-loss in foot and arthritis. Patients in the study found a reduction of around 40% of their pain during the test. This has provided further evidence of the benefits of weight loss in improving foot and ankle pain. To see the Alter G Zero-gravity treadmill working click here
Mr Dawe has been invited to speak to all comers at the Nuffield Chichester on the 30th October. His talk will cover many conditions affecting the foot and ankle such as painful bunions, painful toes, heel pain and the myriad of different treatments available for foot and ankle pain.
Click here to book your place Mr Dawe has been in the news recently with article about him in the Chichester post:
http://www.chichesterpost.co.uk/2018/08/expert-surgeon-joins-hospital/ |
AuthorChichester Foot and Ankle Archives
November 2020
Categories |
|
Oving Clinic
Tel: 01243773167 |
Chichester Nuffield
Private secretary: Sarah Brown Tel: 01243753022 |
Goring Hall secretary:
Nicole Murray Tel: 01903953201 |
Copyright © 2015
- Chichester Foot and Ankle
- Foot and ankle conditions
- Treatments
- Foot and ankle referrals
-
Resources
- Sites of foot pain
- Links to other foot and ankle services and resources
- Internal
-
Rehab protocols
>
- Rehabilitation from achiles tendon rupture treated without surgery using VACOped boot
- Recovery from achilles rupture without surgery using VACOped boot
- Rehabilitation from achilles tendon rupture treated without surgery using Boot and Wedges
- Rehabilitation from achilles tendon rupture treated with surgery in Aircast boot and wedges
- Foot and Ankle rehabilitation



 RSS Feed
RSS Feed

